This has been a tremendously long, drawn out journey since 2005. That is when I began falling with my “spells” which led to more concern and wanting answers. From doctor to doctor, town to town, the doctors would give up or nicely tell me I’m crazy basically. Even the ones who saw my spell in their offices, but I had no proof on any test that they tried. Each time I would question myself, “Is this in my head?”, “Was *** right about I’m just crazy?”, “Aren’t these really happening?”. Even in the last few months, I have questioned myself about my spells. After going so long with no answers and through multiple doctors, it’s nice to finally have a diagnosis. Already diagnosed with fibromyalgia and mild POTS, but now we know the main kicker hopefully.

YES!! You read that correctly!! While at Vanderbilt for testing in November 2018, they ruled that I had borderline POTS. I was so frustrated by this and instantly began crying in the office talking to the doctor. Still no concrete diagnosis. I was over it again! Each time I got frustrated in the past, I would ignore and hide all of my symptoms. God shut that down this time, it’s all effected me worse than ever.
Since September of 2017, I have been unable to drive far (if any) or work. I can barely get out of bed some days, using a cane to walk if in public on the “ok” days. Falling…well the floor and I have became buddies, but my right side (weak side) truly hates the floor. The weight gain from not being able to be active, well I am not happy about it at all! I know when I get strength and these spells gone, I’ll lose it. There are so many other things that goes along with it. Some of my community, family, and friends have seen these spells. It’s so embarrassing, I like to be in control of my body and able to do simple things. I took for granted a lot. Walking. Driving. Getting out of bed. Fixing my hair. Standing in a shower. Simple things from day to day. We don’t realize everything we are blessed with until it’s taken away.
I tend to go everywhere with stories, when I talk and type…sorry y’all.
Here it is March 2019, I decided to look up the Vanderbilt summary of my visit. There it was plain as day conversion disorder known as Functional Neurological Disorder. Several doctors told me it’s like my brain isn’t connecting to my other organs and nervous system correctly. Well once I looked up FND, there it was the exact same thing with a title now. I did my research and joined a few groups on Facebook. That is really where you learn about these disorders. The real people’s encounters are the jackpot when trying to understand medical stuff. I became aware that we share a lot of similarities. I finally have answers!!!!
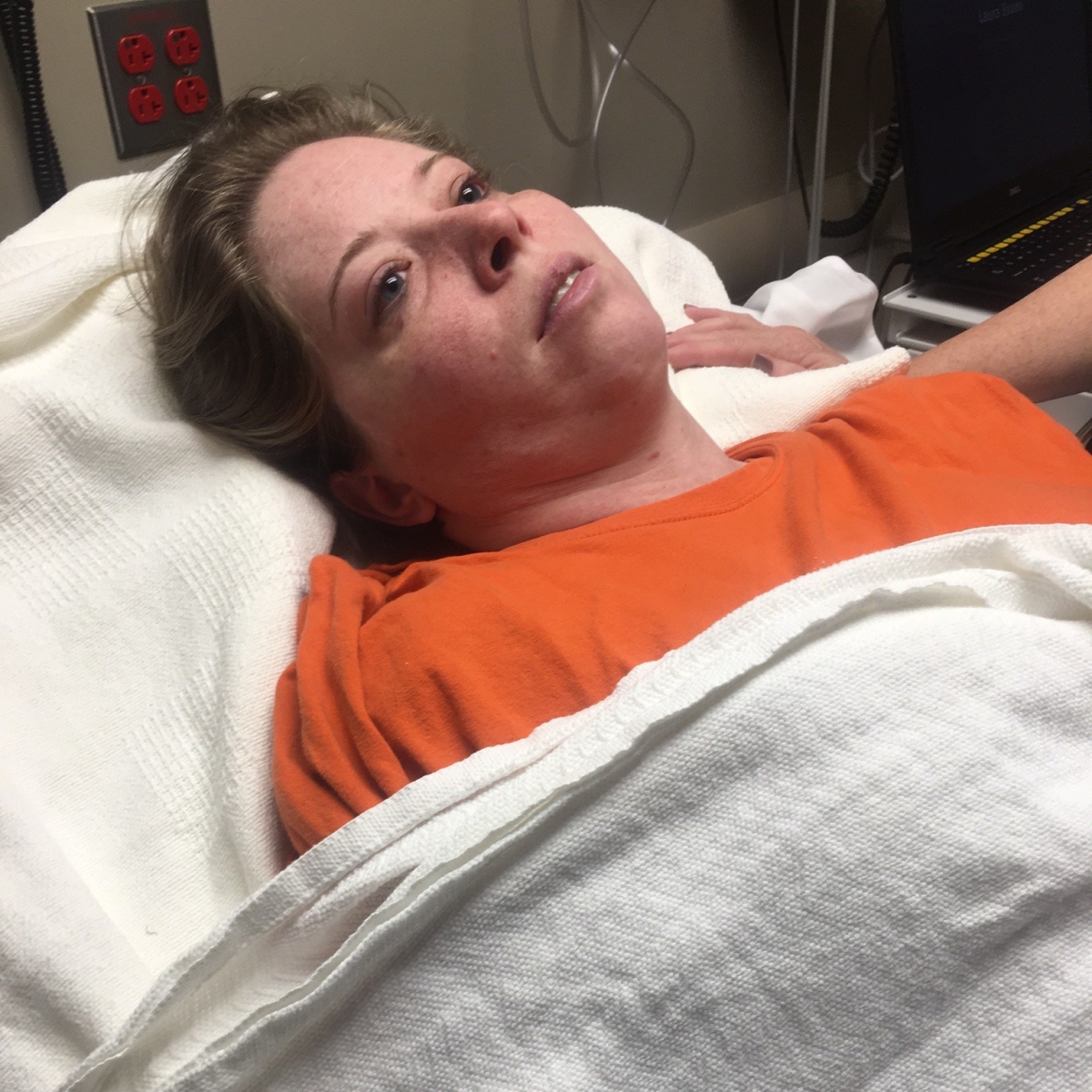
During my senior year of high school, washing dishes after school, my face drooped and stayed for a few seconds. My first thought was I’m having a stroke. Randomly I still have that issue, but my face on the right side droops a little at all times. I wish I knew if it was like that before the first time it happened.

This was a huge find to me about my face. I have always tried to hide it in photos. It was like a confirmation from God, that’s it. My primary doctor has been fantastic and helped me more than anyone. He had already seen the summary from Vanderbilt and booked me cognitive behavioral therapy. I begin the hard and long process to hopefully get my life back somewhat in April 2019.
This was hard at first when I read the diagnosis and looked it up. My first thought was, “It is all in my head. They were right.” Well after researching more, speaking to medical professionals, and hearing others peoples experiences with it, I have no shame of this disorder. It isn’t something I can’t help. If your heart was malfunctioning, you would fix it anyway possible right? My brain is another organ that I need and it’s malfunctioning. I’m going to do all I can to get the help I need to retain it. Support and prays are all I need from you! Any therapy is HARD. Mental therapy will be emotional and draining, finding possibly old wounds or triggers. I got God, family, and you guys as support, so I will make it and NOT GIVE UP.

What is Functional Neurological Disorder (FND)?
Functional neurological disorder (FND) is a medical condition in which there is a problem with the functioning of the nervous system and how the brain and body sends and/or receives signals, rather than a structural disease process such as multiple sclerosis or stroke. FND can encompass a wide variety of neurological symptoms, such as limb weakness or seizures.
FND is a condition at the interface between the specialties of neurology and psychiatry. Conventional tests such as MRI brain scans and EEGs are usually normal in patients with FND. This had led, historically, to the condition being relatively neglected by both clinicians and researchers. However, it is now established that FND is a common cause of disability and distress, which may overlap with other problems such as chronic pain and fatigue. Encouraging studies support the potential reversibility of FND with specifically tailored treatments. New scientific findings are influencing how patients are diagnosed and treated which is creating an overall change in attitude towards people with FND.
Older ideas that FND is “all psychological” and that the diagnosis is made only when someone has normal tests have changed since the mid-2000s. The new understanding, including modern neuroscientific studies, has shown that FND is not a diagnosis of exclusion. It has specific clinical features of its own and is a disorder of the nervous system functioning in which many perspectives are necessary. These vary a lot from person to person. In some people, psychological factors are important, in others they are not.
Signs & Symptoms
FND patients can experience a wide range and combination of symptoms that are physical, sensory and/or cognitive. The most common include:
Motor dysfunction
• Functional limb weakness/paralysis
• Functional movement disorders; including tremor, spasms (dystonia), jerky movements (myoclonus) and problems walking (gait disorder)
• Functional speech symptoms; including whispering speech (dysphonia), slurred or stuttering speech
Sensory dysfunction
• Functional sensory disturbance includes altered sensation; e.g. numbness, tingling or pain in the face, torso or limbs. This often occurs on one side of the body
• Functional visual symptoms; including loss of vision or double vision
Episodes of altered awareness
• Dissociative (non-epileptic) seizures, blackouts and faints: these symptoms can overlap and can look like epileptic seizures or faints (syncope)
Symptoms often fluctuate and may vary from day to day or be present all the time. Some patients with FND may experience substantial or even complete remission followed by sudden relapses of symptoms.
Other physical and psychological symptoms are commonly experienced by patients with FND but may not be present. These include: chronic pains, fatigue, sleep problems, memory symptoms, bowel and bladder symptoms, anxiety and depression.
Causes
The exact cause of FND is unknown, although ongoing research is starting to provide suggestions as to how and why it develops. Many different predisposing factors can make patients more susceptible to FND such as having another neurological condition, experiencing chronic pain, fatigue or stress. However, some people with FND have none of these risk factors.
At the time FND begins, studies have shown that there may be triggering factors like a physical injury, infectious illness, panic attack or migraine which can give someone the first experience of the symptoms. These symptoms normally settle down on their own. However, in FND the symptoms become ‘stuck’ in a ‘pattern’ in the nervous system. That ‘pattern’ is reflected in altered brain functioning. The result is a genuine and disabling problem, which the patient cannot control. The aim of treatment is to ‘retrain the brain’, for example by unlearning abnormal and dysfunctional movement patterns that have developed and relearning normal movement.
One way of thinking about FND is looking at it as a bit like a ‘software’ problem on a computer. The ‘hardware’ is not damaged but there is a problem with the ‘software’ and so the computer doesn’t work doesn’t work properly. Conventional structural MRI brain scans are usually normal in FND unless the person has another neurological condition. Functional’ brain scans (fMRI) are starting to provide early evidence for how the brain goes wrong in FND. fMRI scans show changes in patients with FND which look different from healthy patients without these symptoms as well as healthy people ‘pretending’ to have these symptoms. Functional imaging is still a research tool and is not developed enough to be used in the diagnosis of FND. Scans support what patients and researchers already know – these are genuine disorders in which there is a change in brain functioning, which is out with the control of the person with FND.
Historically, FND has traditionally been viewed as an entirely psychological disorder in which repressed psychological stress or trauma gets ‘converted’ into a physical symptom. This is where the term ‘conversion disorder’ comes from. Psychological disorders and stressful life events, both recent and in childhood, may be risk factors for developing the condition in some patients, but they rarely provide a full explanation for the cause of the condition and are absent in many patients. Patients do not have to be depressed, anxious or the survivor of adverse childhood experience to develop FND.
Modern theories propose that FND has many causes, which vary from patient to patient. One comparison is to think about heart disease. There are lots of causes of heart disease – smoking, genetic factors, diet and even stress-related / psychological factors such as depression. Smoking may be a factor in heart disease in many people, but it is not in everyone. The same analogy can be made for FND. In some psychological factors such as past trauma or stress at the time of symptom onset in FND are important in understanding how the brain has gone wrong. In others the presence of a problem like migraine or a physical injury may be the most important thing.
Affected Populations
The exact prevalence of FND is unknown. However, research suggests FND is the second most common reason for a neurological outpatient visit after headache/migraine; accounting for one sixth of diagnoses. This means FND is as common as multiple sclerosis or Parkinson’s disease.
FND can affect anyone, at any time, although it is uncommon in children under 10. FND is more likely to affect women than men for most symptoms, although when patients present over the age of 50 then it occurs equally in both groups.
(info from https://rarediseases.org/rare-diseases/fnd/)

Thank you for reading and keeping up with my journey.
This is just the first step, accepting the diagnosis.
More blogs to come through this process of recovery.